DIABETIC EYE DISEASE
Diabetes can have a variety of effects on the eye. A common condition, diabetic retinopathy, is one in which the tiny vessels of the retina are damaged. This is a leading cause of blindness in developed countries such as Singapore. The incidence of diabetic retinopathy rises the longer one has diabetes; individuals with diabetes for more than 10 years are more likely to have blood vessel anomalies and retinopathy.
TYPES OF DIABETIC RETINOPATHY
1) Non-Proliferative Retinopathy
Non-proliferative or background retinopathy refers to the early stage of diabetic retinopathy. There are minute blood spots, minor microvascular alterations (microaneurysms), and protein and fat leaks (exudates). There may be no visible symptoms in the early stages.
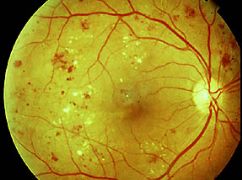
2) Proliferative Retinopathy
As the retinopathy worsens, new abnormal vessels may form on the surface of the retina or the optic nerve (neovascularisation). These vessels may rupture and flow into the eye, resulting in a temporary loss of vision. Scarring and fibrosis may also occur, causing traction and strain on the retina, leading in retinal detachment and vision loss.
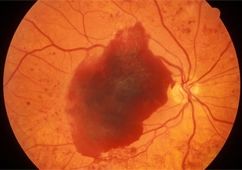
3) Diabetic Maculopathy
Vision may be lost if the macula is compromised and there is fluid leakage and swelling.
EYE SCREENING
Individuals with diabetes should have regular eye examinations to monitor for vision issues. The eye specialist will perform a complete examination, including dilating the pupils to inspect the retina. A fundus flourescein angiography is sometimes conducted to assess the degree and extent of the condition.
EARLY DETECTION TO GET THE BEST POSSIBLE TREATMENT
Most individuals, including diabetics, are unaware that diabetes can have an impact on the eyes. The vast majority of diabetic eye disease patients go undiagnosed and untreated. Diabetic eye screening is helpful in detecting the condition early for immediate diabetic retinopathy treatment.

